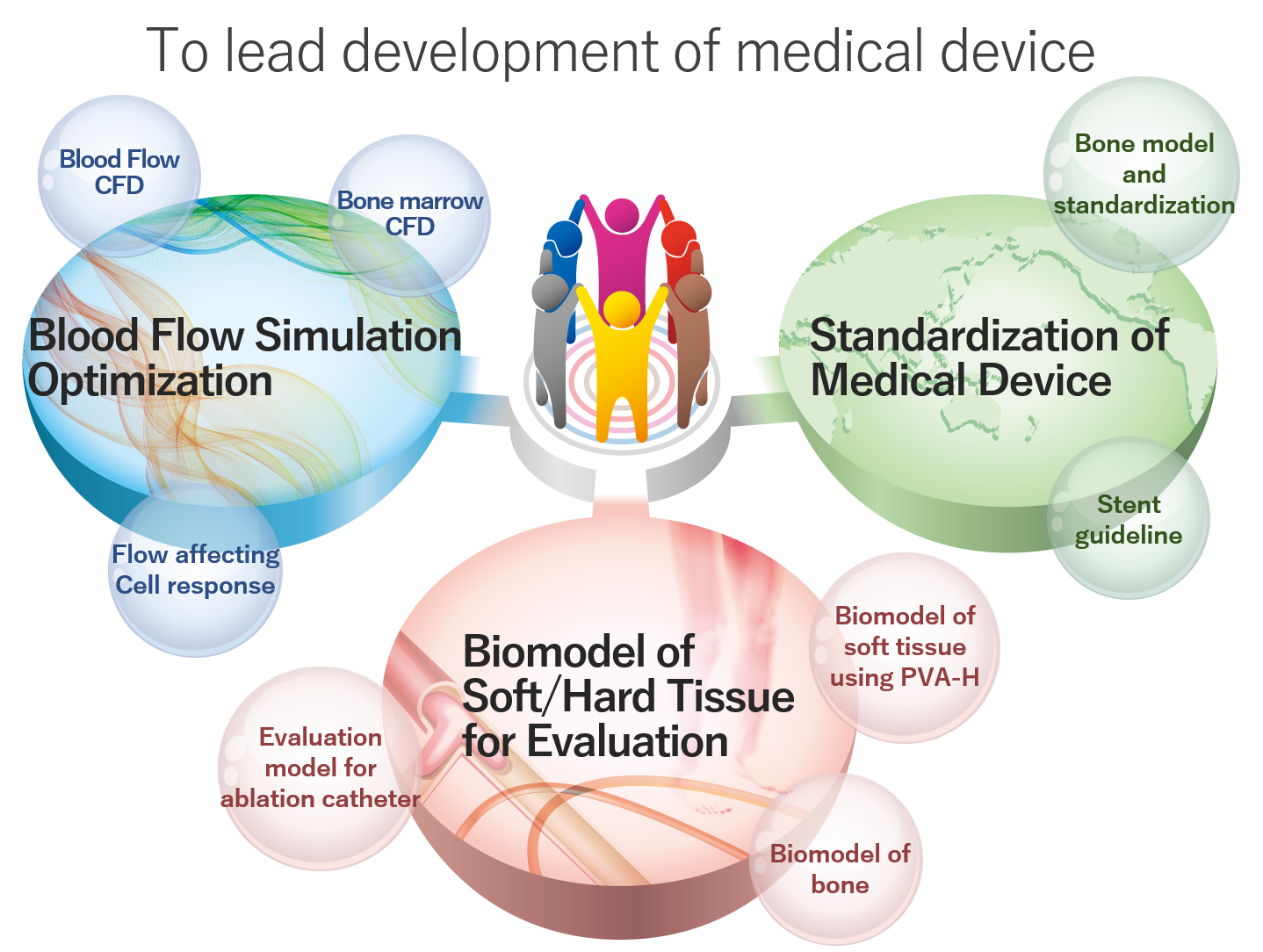
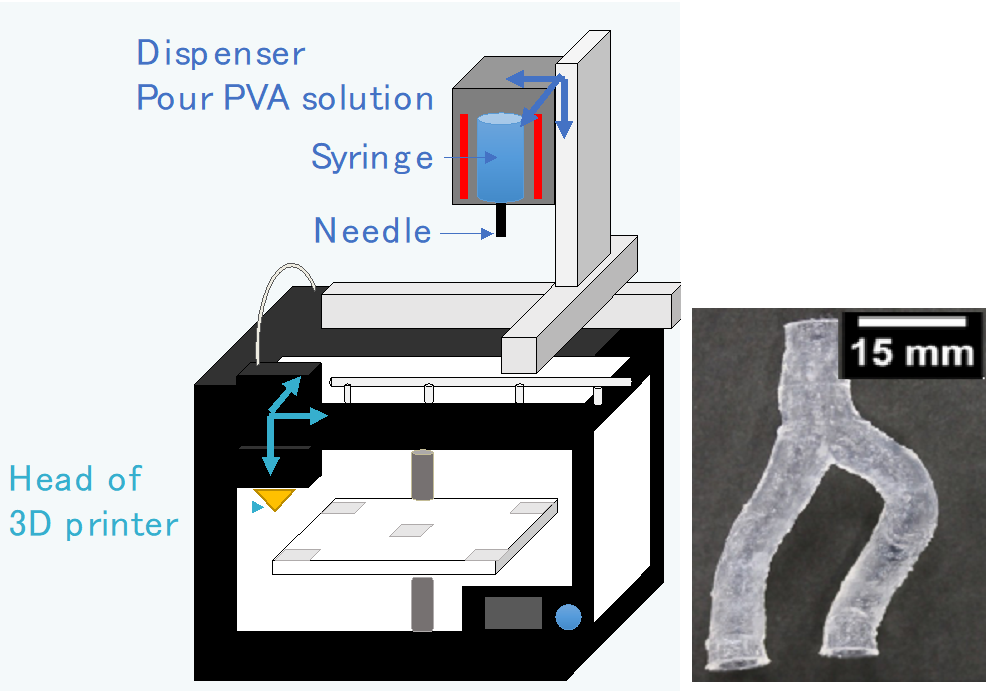
Our lab have developed blood vessel biomodels made of PVA-H for the first time in the world. Since instant fabrication of patiend-spesific biomodels enable checking procedure just before surgery, we are trying to develop "PVA-H 3D printer" as a new method of biomodel fabrication. We are now performing sensory test by doctors in addition to mechanical testing in order to produce realistic sence of use.
Kobayashi, Naohiro, et al. "Development and Evaluation of PVA-H 3D Printed Blood Vessel Biomodels With Several Stiffness." ASME International Mechanical Engineering Congress and Exposition. Vol. 84522. American Society of Mechanical Engineers, 2020.

Ultrasound (echo) machines are used in many medical fields because they allow easy observation of the inside of a body. Biomodels play an important role in the evaluation of newly developed echo machines. The biomodels used for this purpose not only have a shape and mechanical properties similar to those of a living body, but also contain scatterers because the images taken by the machine need to represent a state similar to that of a living body. In addition, it must be transparent so that medical devices such as catheters inserted into blood vessels can be seen from the outside. We are developing a model that satisfies both of these requirements.

Intervascular treatment use stents which expand the cavity of blood vessels or change the vascular flow. Blood clot and re-blockage sometimes happen after treatment with stents. Covering stents with endothelial cells may help to avoid re-blockage. Thus, we are trying to reveal the effects of flow along with stents and surface treatment to endothelialization. We perform in-vitro experiments with cultured cells and CFD simulation.

Angioscopes are medical devices used to analyze and evaluate the properties of blood vessels for diagnosing diseases. They are placed within blood vessels to directly observe the shape and color of the blood vessel wall. To do that, a transparent fluid called flush is released from the tip of a catheter to clear out opaque blood. However, due to the effects of flush on the body, the amount of available flush is limited, and as such the blood vessel wall can not be observed. Therefore, we propose optimal flushing conditions through CFD analysis to investigate the effects of flushing conditions on the angiography visibility.

Human society has been facing various infection diseases. In case of COVID-19, virus from infected patients spreads through the air and cause droplet infections. In response to world-wide spread of infection, computational simulation have been performed to visualize how droplets spreads around human body. On the contrast, inside the body, there are still many unknows on generation mechanism of droplet. Therefore, we performs computational simulation of fluid dynamics on human airway to analyze and visualize how and how many droplets are generated.
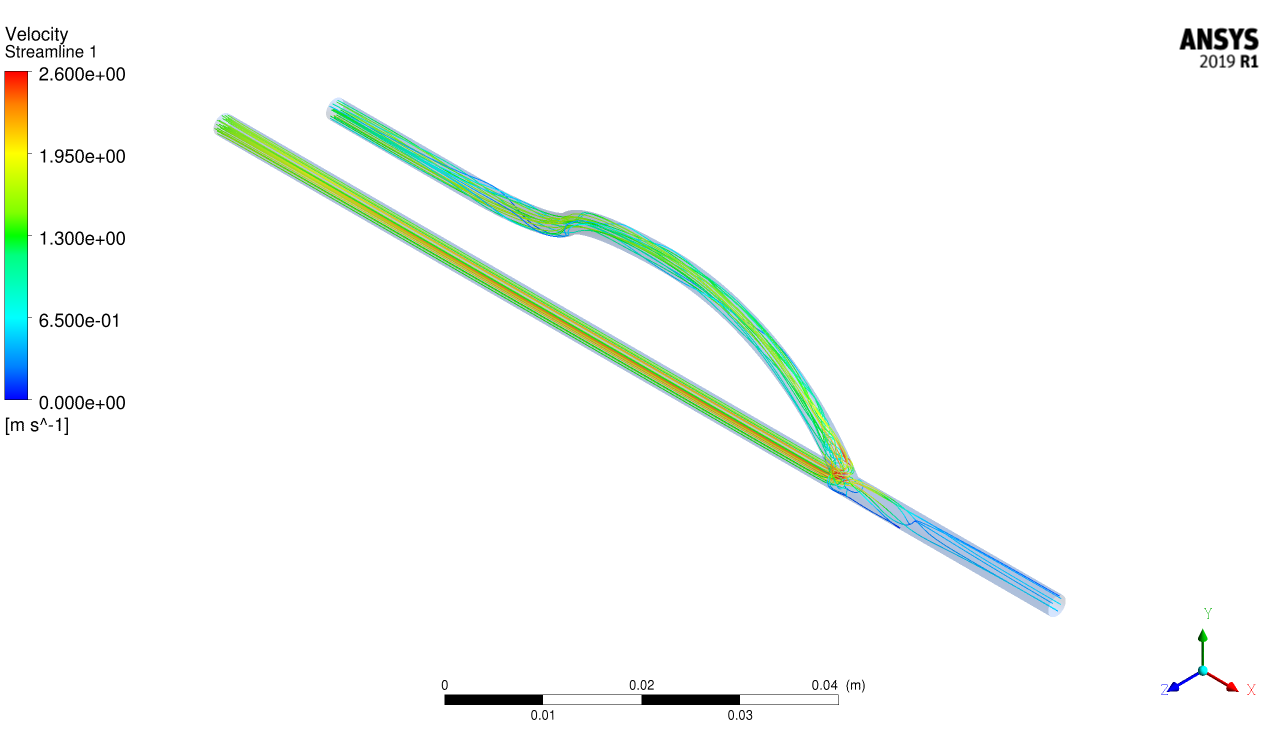
Hemodialysis is the most popular medical treatment for kidney failure. More than 300,000 patients take hemodialysis in Japan. When we conduct hemodialysis, around 200 mL/min (※) of blood will be drawn from the patient’s forearm. Generally to say, however, such amount of blood doesn’t flow in the vein of the arm. To pump enough amount of the blood into the dialyzer, surgeon will place an unique blood vessel named arteriovenous fistula (AVF) in the patient's forearm. AVF is the blood vessel whose vein and artery are connected through the surgery. After the placement of AVF, much blood from the artery flows into the vein. Then, we can get enough amount of blood from the vein. However, the AVF will cause the abnormal blood flow in the connected region (anastomosis region), and this flow leads to the onset of stenosis in the anastomosis region. The stenosis may make it difficult to continue the hemodialysis. So it is important to decrease the onset of stenosis. Our research aim is to propose the optimal geometry of AVF to avoid stenosis. CFD analysis and visualizing the condition of blood flow in AVF will help to find a proposal of AVF geometry.
※ This is the value adopted in Japan. The value is variable depending on the country.
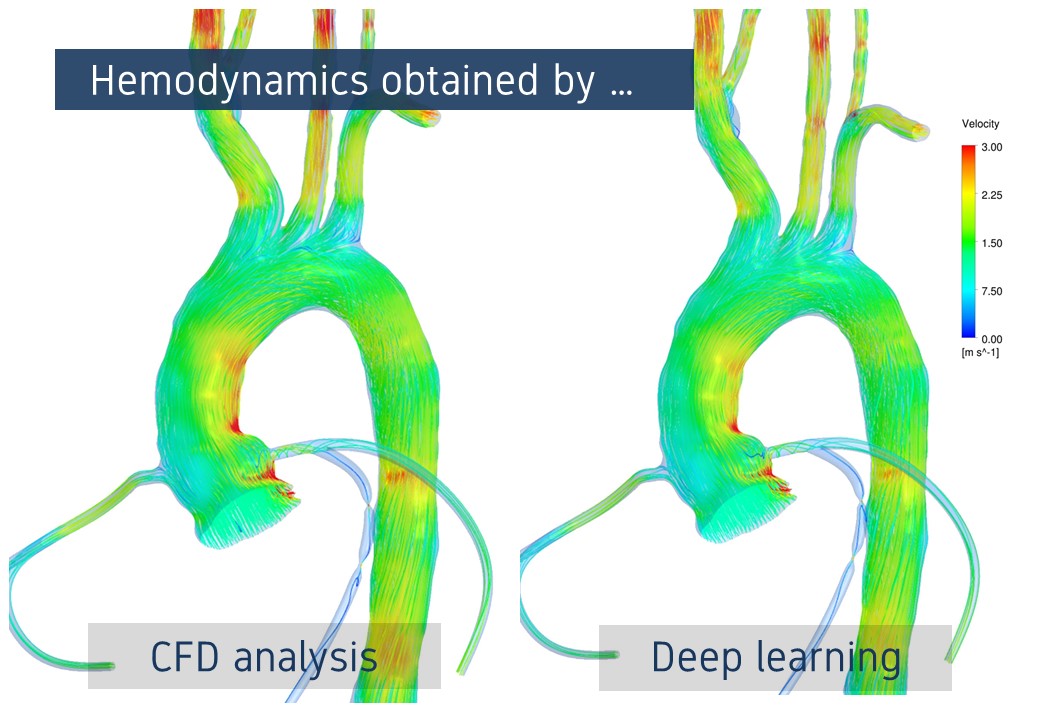
To know the flow field in the blood vessel is gathering attention to be useful for treatment and prediction of disease. In previous days, blood flow measurement using medical devices on patients and Computational Fluid Dynamics (CFD) analysis using computers mainly have been conducted. However, measurement has a limitation for the resolution and CFD analysis has a problem of long calculation time. In other to solve these problems, we use deep learning technic instead of CFD, and we are developing a new technology that instantly estimate the flow field for the vascular geometry constructed from medical images with a resolution as high as that of CFD analysis.
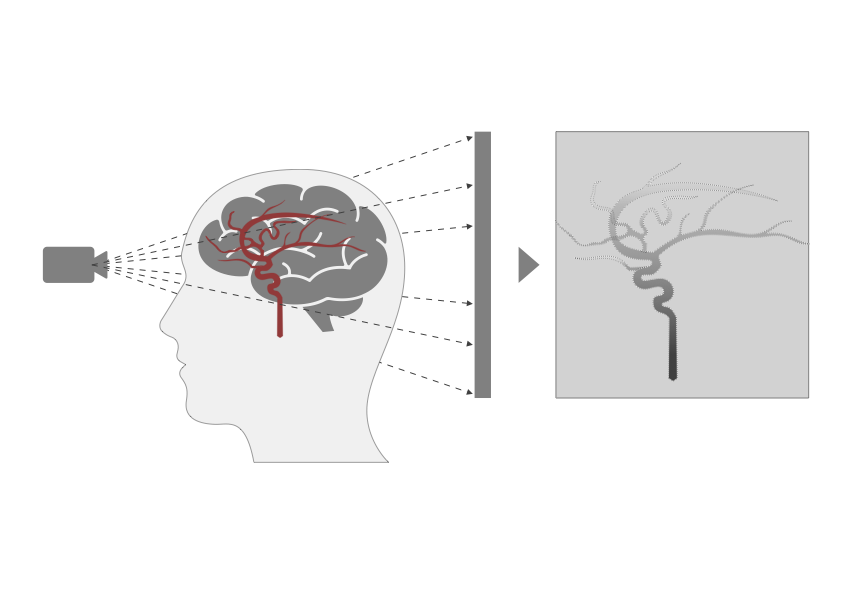
We are working on a hemodynamics estimation using medical images to obtain the 'real hemodynamics' in a patient. In the current clinical situation, medical doctors are guessing hemodynamics in a patient by observing medical images, but in research fields, quantitative hemodynamics estimations are becoming possible with medical images and some image processing techniques. Previous studies have proposed several image processing techniques to detect movements of blood flow from the medical images. As the target medical images also vary to several types in response to the image acquisition conditions, we need to investigate the proper combinations of the image processing techniques and the medical images. However, investigating those combinations requires a variety of medical images, which is difficult. We are computationally simulating medical images to enable investigations on those combinations. In the future, a quick and proper hemodynamics estimation will be possible only from medical images and their conditions. Our final goal is to provide the appropriate hemodynamics to medical doctors in clinical situations.

Risk evaluation of vascular disaeses is showing its importance. Many of the previous reserches have shown that the manifestation of the disease is correlated to the hemodynamic situations. However, it is not easy to achieve those information. That is why we turned our view onto the vessel shape and studying on the risk evaluation based on geometrical researches.
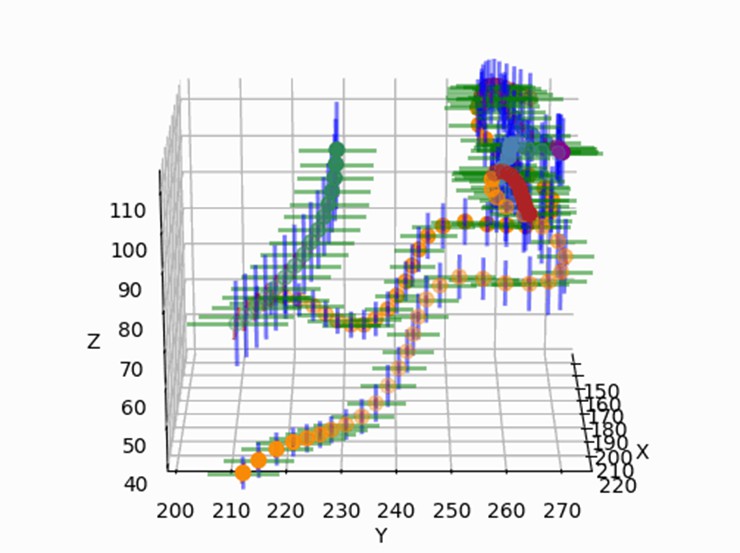
"Disease" indicates the state of "not healthy," but what kind of state can be thought as "healthy"? Changes in blood vessel geometry are often used as a description of disease state. To evaluate this shape change quantitatively, we propose a "standard cerebrovascular coordinate system" which expressed as the average and variation of blood vessel runs (position and diameter) in human brain. By defining a uniform reference shape of blood vessels, "the difference from coordinate system" can be calculated as a quantitative criteria for disease diagnosis and medical device selection.